A new generation of drugs is emerging in the field of transplant medicine, with the potential to change how we approach organ and cell transplantation for type 1 diabetes.
One of these drugs is Tegoprubart, an experimental immunosuppressant designed to protect the transplanted organ while causing less harm to the rest of the body.
This potentially groundbreaking therapy has already attracted attention through Katie Beth, whose post about her so-called “remission” went viral online.
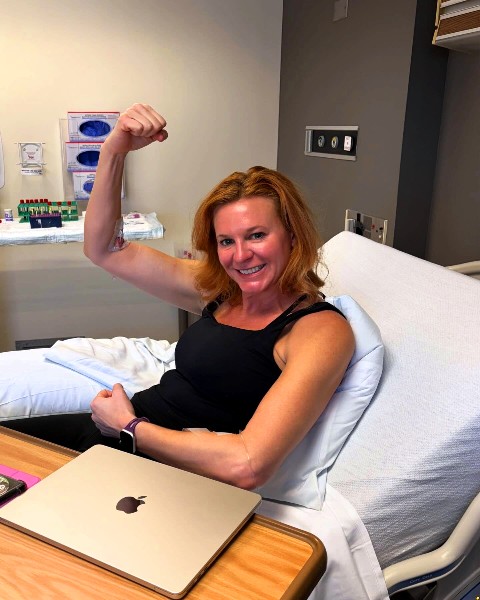
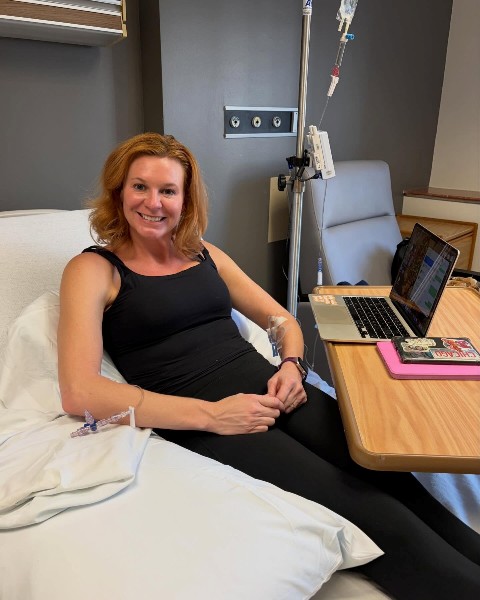
Katie Beth has type 1 diabetes and underwent a stem cell transplant in Chicago about a month ago. Today, she no longer requires insulin, but she is taking the experimental immunosuppressant.
Why are immunosuppressants necessary?
The body recognizes transplanted tissue as foreign and attempts to destroy it. To prevent organ rejection and allow the graft to function long-term, patients must take immunosuppressants. In the case of pancreas or islet cell transplants, this protection enables life without insulin.
In other words: without immunosuppression, most of today’s transplant-based “remissions” of diabetes wouldn’t be possible.
Problems with older drugs
Traditional immunosuppressants such as tacrolimus and cyclosporine have been effective but carry significant side effects. Long-term use is linked to kidney toxicity, increased cardiovascular risk, metabolic complications, and potential damage to beta cells themselves.
The paradox is clear: therapy that protects a transplanted organ can simultaneously stress the very body that needs that organ to function over the long term.
Tegoprubart: A New Immunosuppressant for Safer Diabetes Transplants
Where Tegoprubart fits in
Tegoprubart belongs to a newer generation of biologic immunosuppressants targeting specific T-cell activation pathways (CD40/CD40L).
It was developed with clear objectives:
- Prevent graft rejection
- Avoid the kidney toxicity common with older therapies
- Preserve beta-cell function and metabolic stability
Early clinical results are promising—transplanted organs maintain stable function with a safer profile compared to older drugs.
Why this matters for diabetes
The greatest potential is seen in:
- Simultaneous kidney and pancreas transplants
- Islet cell transplants
- Future stem-cell beta-cell therapies
All these treatments rely on long-term immunosuppression. Making it safer and more tolerable could expand access, allowing more people with diabetes—not just a highly selected few—to benefit.
If you are interested in this topic, you can also read our article:
Do we even want therapies without immunosuppressants?
Absolutely.
The ideal future includes encapsulated cells, gene therapies, and immune tolerance without chronic medications.
However, many functional “remissions” currently exist—including pancreas and islet cell transplants—still reliant on immunosuppressants.
Development is therefore moving in two directions: creating therapies that require no immunosuppression, while simultaneously developing safer, more precise immunosuppressive drugs. If the latter become safe enough, transplant-based treatments could become a viable option for a much broader population.
Conclusion
Tegoprubart is not yet approved for routine clinical use, but it clearly signals the direction of transplant medicine—toward precise, safer immunosuppression with fewer side effects and better protection of graft function.
While we wait for therapies that eliminate the need for immunosuppression entirely, this new generation of drugs may make transplant “remissions” more accessible and sustainable long-term.