“Nothing happened, but it almost did.
I carry that with me, in almost every step, in every breath.
It is hard to figure out how to live with that grief.”
My daughter Shai wrote those words. Like her, I struggle too.
Jax was 10 years old, and in our house the rule had always been simple: when your blood sugar is low enough, you can have a fizzy drink. That was the general rule for all our children, who were rarely allowed soda anyway. But Jax has diabetes, which meant that sometimes he had to wait until his blood sugar dropped before he could have one.
![]()
We thought that was a reasonable rule, especially because he would probably drink more soda in his lifetime to treat low blood sugar than his younger brother Phineas ever would. We did not think we needed to explain it any further.
Had I not always been his advocate, and the advocate for his disease, constantly saying he could have whatever he wanted as long as he took insulin for it?
Maybe I should have taught him every detail of diabetes instead of waiting until he was older to fully educate him. Why had I not yet taught him about insulin overdosing? Maybe I was afraid that my child, who already had to carry so much every single day, would be frightened by even more reality — by the truth of his own mortality and how closely this disease keeps him to the edge.
His blood sugar had been perfect all day
When he came home after playing football and asked if he could have a Sprite, I said no — he had to wait until his blood sugar dropped.
He wanted his blood sugar to go low so he could get that precious Sprite waiting for him. I had never told him that insulin could be just as dangerous as it is life-saving.
I had placed the tools of survival — and of death — into the hands of an impulsive 10-year-old who often acted before thinking.
Before bed, my husband Kevin checked Jax’s blood sugar and was pleased to see a perfect reading: 6.2 mmol/L. Without additional technology such as a continuous glucose monitor (CGM) to tell us otherwise — it would have shown two arrows pointing straight down, warning us that his blood sugar was falling dangerously fast — we assumed he was fine.
More than fine. Perfect.

Mumbling. That was all we heard.
“Come help me!” Kev shouted.
There was panic in his voice.
For a split second, I was taken back to the night Jasper had a seizure when he was younger. My thoughts froze. I caught myself wondering, Could this be another seizure? Then I pushed the thought away as quickly as it came.
When I entered the room, Kevin asked me to hand him some juice. It was right there on the dresser, so I was surprised he needed my help with something so simple. But he was fumbling around, trying to find Jax’s blood glucose testing kit.
I walked over to Jax with the juice box, slightly irritated that my husband could not handle this one task himself. But the moment I looked at my son, I knew something was terribly wrong.
He would not look at me. He refused the juice. His eyes stared straight ahead with a terrifying, vacant expression.
He suddenly jerked away from me as I tried again, and then he began to shake.
This was not like any seizure I had seen before.
Now I was panicking too.
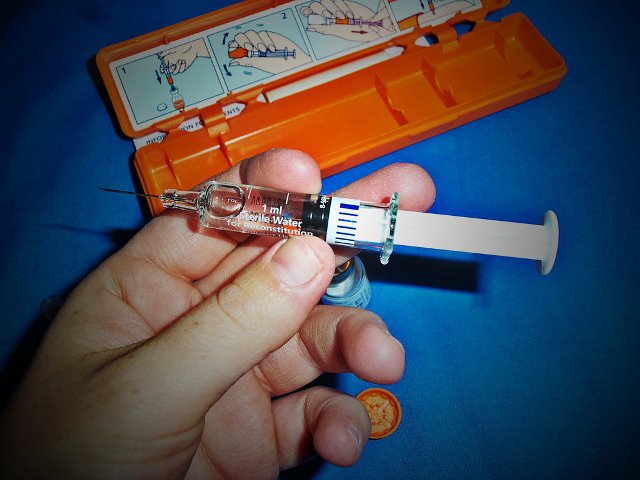
I knew the juice was not going to get into him, even though I kept trying, while shouting at Kevin to prepare the glucagon. Kev handed me the syringe and the powdered glucagon.
And then I fumbled.
I bent the needle.
To make things worse, I kept contaminating the sterile needle by clumsily trying to straighten it with my bare hands. The moment I realized what I had done, I yelled at Kevin to get another one — the spare we kept in the house, in my purse.
I had no idea how much time I had left, or whether there was any left at all.
This was the most violent and devastating seizure I had ever witnessed. I was certain I was watching my son’s final moments.
I had already started grieving him
I did not know how to save him.
I moved much more slowly with the second glucagon kit, even as my mind screamed, How can this be happening? How can I not save him? How can I watch him die?
If there was ever a moment of everything or nothing, it was that one.
I took a deep breath and mixed the glucagon powder with the liquid solution. It seems strange that in a moment of such chaos, such urgency, I slowed down and focused on this one task. My hands were shaking. My breath felt trapped in my chest. Somehow, I managed to fill the syringe with the life-saving mixture.
I was convinced I was already too late.
But I had to try.
I injected it into his thigh.
After the glucagon shot, I tried to hold him with my body. Partly because Kevin was relaying instructions from the emergency operator. But partly because he was so rigid, so tense, and I wanted to soften it somehow. I wanted to hold him one last time while he was still alive, in case I lost him that night.
So I held him on his side, wrapped myself around him, and sobbed.
His body began to tremble as the glucagon took effect. He started moaning and thrashing — and I tried the juice again.
He spat it back into my face.
I knew we were not out of danger.
Maybe he could hear me begging him: “Stay with me, please don’t die.”
I did not know which breath would be his last.
He was that close to death.
We spent the whole night in hospital
He was admitted and placed on a heart monitor and multiple bags of glucose, which had to be changed quickly and repeatedly. His blood sugar kept dropping, and none of us could understand why.
The doctors and I came to the same conclusion: his insulin pump must have malfunctioned.
For a moment, we wondered whether Jax might somehow have overdosed by accident, but we dismissed it. Surely he could not have done that. Surely he would not do that.
In trying to protect his childhood and his innocence, we had neglected our responsibility to teach him how to manage his disease independently. We had avoided the hardest truths and the real dangers, thinking we were protecting him from fear.

Then he told me what had really happened
After I had decided I was going to burn the “faulty” insulin pump and sue the company, Jax finally told me the truth.
He had given himself nearly 16 units of insulin.
I must have looked stunned, because he continued on his own:
“I wanted Sprite, Mom, so I took insulin after you told me I couldn’t have it. And when my sugar still wasn’t low before bed, I took more.”
That was the truth.
Not a pump failure. Not bad luck. Not some mysterious medical event.
A child with diabetes had used the only logic he understood — and nearly died because we had not explained the danger clearly enough.
The diabetic community had warned us
Not doctors. Not nurses. But parents and people living with diabetes themselves.
They had told us to always stay alert. To be careful. To understand that many healthcare professionals do not fully grasp the day-to-day reality of this disease. They told us to check blood sugar twice every night.
“This disease is sneaky,” they said.
“Unpredictable.”
“And too often fatal.”
But that was five years ago.
Today, we have tools that can help predict these events — tools that can save lives before things become critical. If we had had a CGM, Kevin would have seen much more than that perfect 6.2 mmol/L before putting Jax to bed. He would have seen the rapid fall. He would have seen the danger.
But CGMs are expensive, and they were not covered by the Health Insurance Plan.
Families with low incomes, or those surviving on a single income, were forced to live without sensors — or to beg others for help in accessing devices that can literally save lives.
What I see now
As I continue to live with the post-traumatic stress of that night, I now see more clearly just how many people with type 1 diabetes still live in a world where they are misunderstood, overlooked, and left behind.
It is hard for me to accept that the governments in most countries only recently began covering life-saving prescription medications for people with diabetes.
I look at the future and wonder how I will keep my son alive when he grows up and moves away, when I can no longer check on him twice every night.
We invite you to also read our article "Once again, a child with diabetes faces discrimination in kindergarten!"
Once again, a child with diabetes faces discrimination in kindergarten!
Adapted from an article originally published by Beyond Type 1.



